fig2

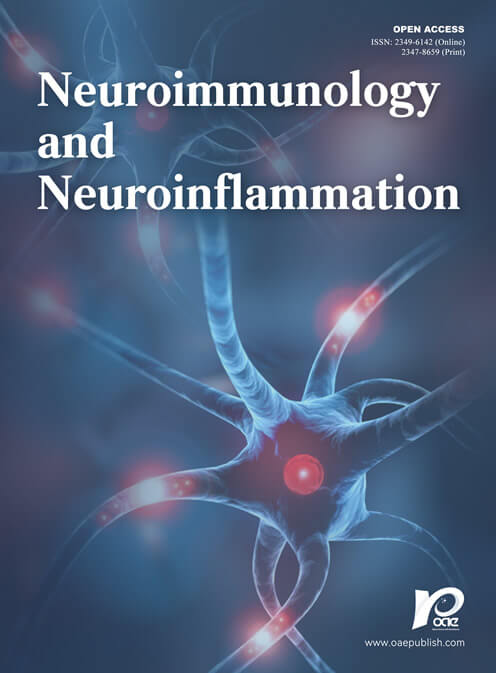
Figure 2. Schematic view of the role of immune cell types in cytokine production, neuroinflammation, and tissue repair. In the early stage of around 24 h, macrophages infiltrate the injured brain and are activated through the TLR2/4 stimulation by molecules known as danger-associated molecular patterns (DAMPs) from necrotic cells. Thereafter, infiltrated macrophages produce inflammatory cytokines and mediators which increase probability of ischemic encephalopathy and blood brain barrier (BBB) destruction. At this stage, macrophages become M1-type inflammatory macrophages. Further on, IL-23 and IL-1β from inflammatory macrophages stimulate IL-17 production from infiltrated γδT cells. After day 3, macrophages are converted into M2-type repairing macrophages which are involved in clearing DAMPs, resolving inflammation, and tissue repair by producing neurotrophic factors such as IGF-1. During the chronic phase, a massive T-cell infiltration occurs. Brain Tregs are attracted via chemokines and proliferate in the cervical lymph node (LN) and the brain. Brain Tregs may thereafter interact with various brain cells including that of microglia, astrocytes, endothelial cells, and neural cells promoting neural cell recovery in th process. IL: interleukin; IGF: insulin growth factor